Volume 4
S/P Autograft
Letter From the Editor, 2016 Rubor Volume 4
Dear Readers,
Thank you for taking the time to read the latest edition of Rubor. Our goal is to create a dialogue about the challenges and triumphs of health care and to encourage creative expression among those at the University of Utah Health Sciences. It is clear by the diverse works submitted this year that there exists extensive talent across campus.
In this volume we continue to explore how artistic expressions allow us to reflect on our experiences in science and medicine. Sandra Osborn’s time working in the blood bank leads her to question the intersection of life and death and explores what it means to live. Through poetry, Andrew Martin, Ana Maria Lopez and Heather Curtis explore the interactions between physicians and patients and provide context to these difficult conversations.
Challenging topics in medical ethics are approached with thoughtful consideration and expressed with artistic eloquence. Christine Kannapel comments on the historical practice of, and medical fascination with, preserving anomalous fetuses in jars. Ian Fordham produces an Italian-style sonnet about a rare phenomenon in which abled bodied individuals desire to be physically disabled and explores the controversy of elective amputation of otherwise healthy limbs.
In addition, photographs are featured that capture magnificent scenes along the Wasatch Front. Original collages and hand-crafted pieces are included that illustrate the balance of objectivity and humanism in medicine. Sketches and paintings also beautifully capture artistic emotion. These represent just of a few of many other works of art found within these pages.
I am pleased to present to you this collection of artistic expressions which is a great demonstration of the creative talent found within the University of Utah community. We hope to continue to serve as a forum for students, patients and health care providers to explore the art of medicine.
Sincerely,
Martin de la Presa
Antelope Island

Blood Loss
My first job as a Laboratory Scientist was at the blood bank of a Trauma 1 Center. The blood bank, in all its vampire-associated humor, was situated in Lower Level 2 of the main patient tower. Windowless, recessed in a hollow underground along with other forgotten spaces—mechanical rooms and housekeeping closets—it was a tomb, of sorts. It was a vault for the blood that came packaged on ice, roughly 300 ccs each, deep crimson, packed red cells separated from their plasma, preserved in CDPA or AS-5.
One fridge, 3-5 degrees Celsius, contained over two hundred units of O Positive blood. Two other fridges held the rest—A, B, AB, Rh Negatives. Hermetic freezers, -30 °C, kept the plasma products: FFP, the counterpart to blood, and cryoprecipitate at 10 ccs a bag, to be pooled and given only in the worst of circumstances.
At room temp, an agitator incubator swayed the platelets to keep them from clumping. In vivo, the circulation keeps platelets in motion. Whenever blood pools, platelets release proteins that activate the coagulation cascade, the body’s miraculous way of stopping blood loss and promote healing. Some wounds, though, are too vast, too deep. The body cannot cope.
The blood bank was strategically located below the trauma bays in the Emergency Department and two floors down from Surgery. One shot down the elevator and the nurses got the life-saving products within minutes.
Other departments were not so fortunate. Labor and Delivery was inconveniently two buildings over, too far from the mother who, in delivering her twins, went into DIC and the nurses could not figure out the maze that led them across buildings and into the dungeons. By the time they hung the blood it was almost too late. Raw from the near miss, the administration blamed the blood bank for being inaccessible, unclear in its directions to the staff. Didn’t we know she could have died?
And so, with every patient type and screen, every unit cross- matched, the possibility of death lingered near. True, most surgeries and deliveries went uneventfully, most transfusions required only one or two units. But we also got calls for active MTPs—four units of red cells, two plasma, one platelet, turn round time 18 minutes, repeated for as long as the nurses kept coming or the patient died. Usually, the patient died. A body could only lose its blood volume so many times.
This was in the years just before the cell-saver, when Dr.— was still taking high risk patients for liver transplants. He stopped after one of them used upwards of 70 units right before Christmas. The patient had been too elderly, too weak. Blood was in short supply, always is—
For every unit, there is a donor, willing to give thirty minutes of her time hooked to a 16-gauge needle, willing to drain her own life supply into a sterile bag. She is given a drink, a snack, many thanks afterwards. It takes her body two months, long after the expiration date on the bag of blood, to replenish that which she has lost. Or given rather, gifted to another body in greater need. Or the trash, as it sometimes happens too. It becomes a question of how to best allocate resources.
Who lives, who dies.
That liver transplant patient—he died.
It was one thing to hear about those patients in critical condition, quite another to see them, touch their graying skin. One Saturday, we had fifteen calls for traumas by early afternoon. With only two of us on shift, we rotated going up. The pager vibrated yet again.
T1 GSW ETA 5 min.
It was my turn. I donned the yellow impermeable gown and gloves, grabbed an alias tag, and headed up with the emergency release blood, liability papers cold and damp atop the units. Up on the bay, the trauma team waited.
Self-inflicted, they said. Missed. Unsuccessful attempt.
The paramedics wheeled in a man, naked on a stretcher. His jaw was gone.
Once inside the bay, the trauma team took over. The head doctor asked for readings, directed treatment. Epinephrine. Intubation. I rushed in to band him around the ankles, give him a name, ZZZIM Mountain or something like it. His feet were the color of ash. Blood? Two units now.
Prepare for surgery. Beeping sounds. Voices calling numbers, medications. People going in, coming out. Papers. Tubes. Instruments. I watched for the inguinal draw. A frantic rush. Then the head of the trauma team called it. Every effort ceased.
I grabbed the unused blood, left the afternoon sunlight that came in through the glass walls, and went down into the darkness and isolation of the blood bank. I sunk in my chair, gown and gloved. This wasn’t the first time I had seen somebody die. I had seen other traumas; I was in the room when my grandfather passed. I had counted the seconds between his slowing breaths, counted for the breath that never came. My grandfather used to say, “When I die, don’t bring me flowers. Give me flowers now, when I see their colors, smell their fragrance. When I die, don’t cry, don’t wear black, don’t bring me flowers.”
Dying is part of life. Death is not.
Eventually, I took off the gown, dropped it into the biohazard laundry bin. I put away the emergency release blood, filled the paperwork. I worked on other type and screens, cross-matches. At the end of my shift, I went home.
I petted my dog for a long time that night. Days in and days out, the years went by, and I would witness others dying, but still would think about that man. I never found adequate answers to my questions.
We worked to save the life he did not want.
At the Heart of VF
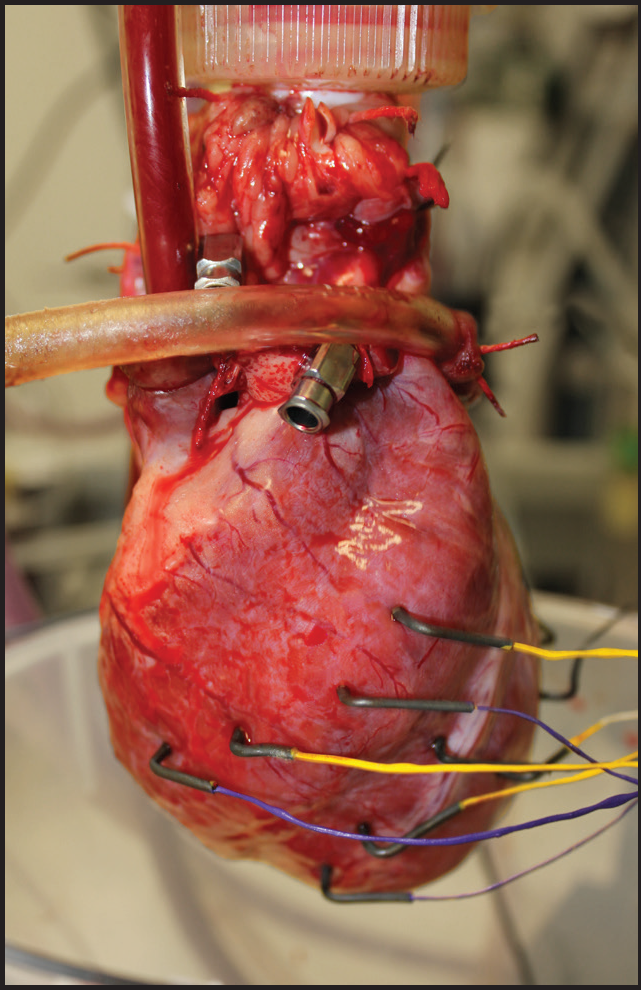
Chest Pain
What does your chest pain feel like?
What do you mean you can’t describe it?
Is it stabbing? Aching? Burning? Squeezing?
Like an elephant sitting on your chest?
Worse with activity?
Better with rest?
Uh-oh.
Now I’ve said too much, and you took the bait.
Now we have to bring you in
And thin your blood.
We’ll do some expensive tests,
And ultimately thread a wire from your groin to your heart
And we’ll probably leave some hardware in one of your arteries.
You may even need open heart surgery.
Is that what you want?
So let me ask you again.
What does your chest pain feel like?
Hidden

Chitenge: Touch Between Mother and Child
We Are His Hands
Response to the Fetuses in Jars
(The Hunterian Museum: the Royal College of Surgeons of England)
I. Prevention of the Unborn
Beginnings with Mercury
sheep skin and silphium,
a match to
dismember
for lovemaking.
A woman’s body, handled
and torn, swollen from
birthing
wishing for rest and pleasure.
A child’s lips- milking
endearing,
but the cause of age,
as one splits into three.
II. Termination of the Unborn
The product of
otium lovemaking
and the investigations
of the intellectual
mind
Children never meant
to live.
One, encased in glass, now a
specimen, collected by
surgeons- a natural death,
a stillbirth, a miscarriage
(blamed on the mother,
thoughts wanton or chaste).
Another,
wrapped in the uterus,
swimming in a pool
of unwanted water,
methods of removal
then plunged into the
walls of tissue and
consumed, ripped, torn
-a method of birth control,
when not a remedy for
predicted death,
the taking of a life.
Buried into the ground,
or burnt to ash,
preserved in a jar.
Silent Teacher
Rooms with steel and fans
Chemically fixed tissues
His last gift demands
Structures framed
Language of topography
Everything is named
In life a good man
An honored teacher in death
Lessons to expand
Terminal
15
Am I going to die?
Well,
It’s hard to say.
So many factors.
We’ll know more when
38
What will I tell my children?
There are resources.
There are folks,
experts,
You are not alone.
61
Why couldn’t it be me?
We always thought
I’d be the first
to go.
I don’t want her to be alone.
84
I’m dying.
We’re all dying.
I’m just a little closer to you.
Nervous laughter
Present silence.
Radical Mastectomy
Silent Dancer
Severed Ties
To lose a limb, anathema to me.
Yet once I thought how simple it would make
my life inside my mind, to give, to take,
a limb away; a crippled man I’d be.
But whosoever really thinks they see
façade in me; that I am just a fake,
I castigate and leave you in my wake
for I have all the reason not to bleed.
To part the skin and take a limb away,
means sacrificing all I’ve loved and dreamed,
insulting those whose wounds are here to stay,
I’d burden all my friends, or those who deemed
me worthy of their time; that is to say,
I’d cut away both flesh and friends esteemed.
Both Broken
First Code
She was a new mother.
She gave birth this day.
Post-partum hemorrhage.
Ten units given.
Bleeding controlled.
Transfer to ICU.
I go to meet my patient.
She is intubated to help her
breathe.
Her pulses are thready, almost
imperceptible.
A pool of blood escapes her legs.
She is bleeding again.
We call for OB.
We start fluids.
More blood.
A central line.
Check for pulses.
They are gone.
First Code.
Resident starts chest compressions.
Attending leads.
I check pulses.
2 minutes.
My turn.
I stand on a stepping stool.
Put my hands on her chest.
Up.
Down.
Up.
Down.
Compressions.
2” deep.
The rubber of her chest contracts
beneath me.
Up.
Down.
Are her ribs broken?
Up.
Down.
1 1/2 minutes pass.
Up.
Down.
100 times a minute.
I’m getting tired.
Up.
Down.
2 minutes are up.
I switch positions.
Code continues.
I watch the up and down.
We are her beating heart.
Can we save a life tonight?
Up.
Down.
Pulses restored.
Pressors are running.
More blood.
Transfusion stat.
Fluid bolus.
Emergent hysterectomy.
Rush to OR.
New admit.
I leave to meet my next patient.
I finish my admission.
Tidy up my notes.
No update yet from OR.
It’s late.
Time for home.
I leave the ICU.
I recognize him.
I saw him say goodbye to his wife,
my patient.
I saw him say goodbye as we left for
the OR.
I walk past him.
He is in that space between patient
and stranger.
We have not met.
I have not had an update.
I double back.
Eye contact.
Mr. Morrison?
Yes.
I was following your wife in the ICU.
Do you have an update?
How is she?
She’s dead.
It hits like ice to my chest.
I gasp.
My hands rush to cover my mouth.
His hands rush to cover his own.
Somewhere between patient and
stranger.
For that minute we stand.
Somewhere between doctor and
stranger.
We look into each other’s eyes.
Somewhere in between new life
struck death.
Now simultaneously we embrace.
We hold on.
The minutes pass.
Somewhere between patient and
stranger.
Somewhere between doctor and
stranger.
Somewhere new father now
widower.
I don’t know why these things
happen I tell him.
I don’t know he says.
And we let go.
My tears are pouring.
Do you need someone?
My friends are here.
Thank you.
And we walk away.
New city.
New hospital.
New halls.
The tears don’t stop.
New life.
Fresh death.
Her pulses were thready, almost
imperceptible.
Was I wrong?
Compressions.
2” deep.
The rubber of her chest.
I was her beating heart.
I could not make it beat.
First Code.
To See the World Through Both Eyes

Oil on canvas
The Heart of Medicine
Two hearts cast in aluminum as a symbol for the delicate balance a physician
walks in medicine. The anatomical heart serves to exemplify the core
objectivity essential in the practice of medicine. The heart symbol represents
the humanistic approach and is the framework in which objectivity can
properly function. Each heart is incomplete without the other in the practice
of the art of medicine.
Leather Belt
Take a Sad Song and Make It Better
Learning to Give
Branch Hanging
We carry biases with us. They reflect our backgrounds and what we have been exposed to in our lives. Anchoring bias weighs us down and shapes our approach to others. It is the hope that through acknowledging our biases and moving away from them allows, we can achieve more present, connected interactions with others. This project aims to be a meditation on the possibilities for growth through shared human experience. Just as we are shaped by our biases, so is the wool pulled and shaped by the brass weights. The progression toward stronger connections is represented in the path from soft wool to manila rope to a wooden branch, as the hanging moves from the bottom to the top. An unbiased approach to patients and others is a life long goal, and as such the project is left unfinished. The knitted rope has not been casted off, but rather is left on the branch, with excess rope coiled at the top left of the hanging.