Volume 8
Pathogens: Our Best Frenemies
Novel Human Illness
Everything is quickly changing
Social lives are rearranging
Stopping time will not contain it
Staying in may help us tame it
Butterflies continue flying
Right above the panicked crying
Some of us may think we’re special
But this illness proves us reckless
Many make their efforts known
Some act only for their own
While a certain, careful few
Day by day they grow –and you
See them shining from the trenches
They keep rising from the benches
Say it’s time to face the game
Which itself is the wrong name
For what’s happening among us
Is no game or trick to fool us
But a tragic realization
That we’re mortal and need saving
To the Beloved, In the Cadaver Lab
See my cadaver-body strung prone.
Unzip my canvas for dissection. Lean
across my red-string muscles. Your power
a scalpel. You, so near my anatomy.
Dig and touch my twelve true ribs, the nineteen
bones in my hand. Give them names.
Make me Latinate. Make me like all the others,
common mankind. I am past wounded.
Take your time with me. You know I used to sing.
Wild Child
Pieces of My Heart
“Sewing and quilting have been a part of my life since I was seven years old. My mother started to teach me because her mother had taught her. Through the years, I developed those skills, becoming a teacher and designer. Each and every project utilized the same basic skills, but regardless of the project or student, they were all unique and required trying new things. Medicine is similar. Much of what is taught occurs from an experienced physician to a novice. As experience is gained, many of the daily tasks require the same basic skills, but the need to continue to improve and better care for your patients continues to push you to try and learn new things.
In my nearly two decades of learning new sewing skills, I had never learned a technique called paper-piecing. This technique is considered to be an advanced technique used to create sewn objects with many pieces of various shapes. Without the skills that I have honed over time, I would have failed in attempting this technique for a project. Because it was a new technique, I asked a fellow seamstress to explain the basics to me. Once she did so, I attempted the technique on my own, making many mistakes along the way, but improving and becoming confident by the end of the first section of the heart quilt. Two weeks later, I was able to help my own mother, an avid paper-piece quilter, continue to refine her own skills. I realized that this mimicked the method of education in medicine—see, do, and teach.
The quilt increases in meaning based on the materials that were chosen. There are four generations of fabric. The first is a piece of fabric that I inherited from my grandmother. My grandmother was a force to be reckoned with, receiving a college education in an era where women did not. The second is fabric from my mother. The third is the fabric that I bought for one of my first solo design projects. The fourth-generation fabrics were all used in projects for various nieces and nephews. These fabrics are different fibers, different weaves, and different weights, increasing the difficulty of the project. Regardless of the background, each fabric was an essential part of the quilt.
I had hoped to learn paper piecing. I not only learned that skill but learned that medicine, just like sewing, is based on heritage and the desire to improve. This project, just like the art of learning medicine, was not easy. Mistakes are made, it takes time, it takes effort, and it has physical tolls. But, the benefit far outweighs the difficulties. This quilt symbolizes the many different facets of medical education and of being a physician.”
Fallen Through the Cracks
We did the exam, gave her the news and she was silent.
Did she understand? I thought.
Latina female, Spanish speaking.
it’s OK we speak her language.
Her face was still, unchanged from the beginning of the encounter.
Minutes before, the young woman in front of me was telling me her story.
She was talking and talking in circles filled with pain
And desperation.
Something wasn’t right.
I felt it in my stomach as a nervous tickle.
But her face was still so stoic.
Why am I nervous? I thought.
My preceptor greets us in the room. I was taking too long, again.
As she is speaking my mind wanders and I see myself in that chair, I see my friends and my peers.
And I am angry and sad, or is it shock?
Why is she not angry? I thought.
Does she understand? I thought again.
It’s anger.
Why am I angry at her when it is our system that failed her?
Pap smear 2 years ago: HPV +
Colposcopy results 2 years ago: HSIL, cannot rule out invasive disease.
Then nothing.
Pelvic exam from today: too heartbreaking to be included.
There has to be a reason.
I am frantically scrolling through EPIC in search of a reason. Maybe a reason to blame her?
Just any reason. I thought.
Numerous visits with the same complaint over the years: severe diffuse abdominal/pelvic pain.
“Most likely functional;” “anxiety related;” “undiagnosed” appear on the screen.
She should be furious. I thought.
Her face was still, unchanged.
She is a single mom. I remember. What will happen to her kids? I dare to think.
Cervical cancer is supposed to be the cancer you “should never have to get.”
Screening works.
It’s the cancer you don’t get. I repeat, trying to convince myself.
But she got it. And she was alone. And she is alone. And she is my age. My age.
The visit ended. Just like that.
A deep breath and I move in slow motion to the next patient room.
Before I knock we cross paths as she makes her way toward the exit.
And I see the slightest sparkle reflect off of her eyes.
She understands. I thought.
White Coat Blues
White coat blues,
got them white coat blues.
My coat is so darn heavy,
Something in every pocket,
that when I put it on,
my neck pops out of socket.
White coat blues,
got them white coat blues
My coat has got some colors
that certainly ain’t white.
Not sure when they got there,
and that just don’t seen right.
White coat blues,
got them white coat blues.
My coat is stained with coffee
And there’s vomit on my shoes.
Oh, you want to slow down?
Like that’s something you can choose.
White coat blues,
got them white coat blues.
There’s a sweat ring roung my collar
and dark rings round my eyes.
You talk about the weekend,
and a part inside me dies.
White coat blues,
got them white coat blues.
My coat smells like a gym sock.
I won’t apologize.
They only bought us one this year.
They ran out of supplies.
White coat blues,
got them white coat blues.
My coat keeps getting older
And so, I guess, do I.
A sobering thought enough
that also molifies.
For when I’m an attending,
in not so much time now,
I’ll have at least two white coats,
and they’ll be clean, I vow.
The Way I See It: What Doctors Name Their Fish
The Way I See It: Intubate
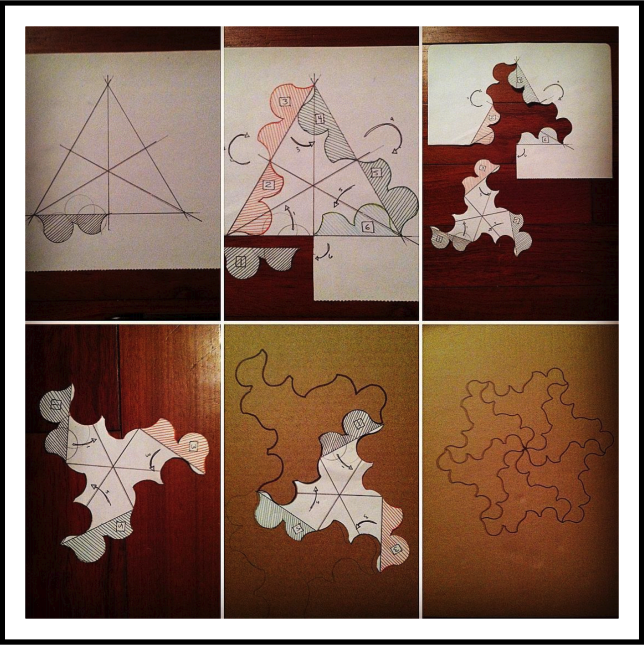
A Study of Tessellation
Focus on the Numbers
15: the number of feet you flew through the air in the incident; the number of days later I’m still thinking about your case.
9: the number of pieces your skull was in when you arrived; the number of upbeat songs I played in my car during my drive home.
5: the number of months you were alive; the time in the afternoon I called my mom, desperately needing to talk about it with someone.
2: the number of caretakers who should have protected you, but didn’t; the number of times I had to fight back tears during your autopsy.
1: the number of blows you received when you wouldn’t stop crying; the total number of post mortems like yours I hope I’ll have to see in my life.
Headlights
“So, how did you get into medical school?”
I have been asked this question in a situation that I had only beforehand seen on social media. We are in the middle of a modern-day Civil Rights movement, of which the tipping point was the murder of George Floyd. This event brought me back to the evening of September 19, 2019. Around the same time, there were many events reporting people of color for doing everyday activities. There had also been many police shootings where suspects were shot dead for acting “suspicious,” such as the shooting of Philando Castile back in 2016. I had a plan if I were ever racially profiled by the police. However, I never actually thought I would ever have to use it, especially after getting accepted into medical school.
My journey started years ago in Southern Mexico. I was raised by a strong, resilient, single mother who did everything to bring me up the best way possible, despite our difficult circumstances. When I was 12 years old, we immigrated to Utah for a better future. I had to learn to adapt to a new culture, language and system. I did not know how to fit in, so I thought I needed to do what other Mexican immigrant kids were doing and join the gang culture. I felt that society expected it of me. Fortunately, my mom and stepdad served as my moral compass and taught me the importance of making the right choices to reach my potential. As I increasingly focused on my academics and school involvement, my path diverged from the gang culture into one of endless possibilities. I found academic and community success as an Eagle Scout, Sterling Scholar for French, and even became a high school honors graduate.
When it was time to go to college, I realized that my immigration status would not provide me the same opportunities that my peers may take for granted. I found out how to get in-state tuition and obtain the necessary private funding because I was not eligible for FAFSA. In the end, I decided to prepare to apply to medical school despite my immigration status. An opportunity appeared in 2012, with the passing of the Deferred Action for Childhood Arrivals (DACA), which allows individuals brought to the United States as kids and remained undocumented to get deportation deferral and a social security card for employment. Despite the threat to terminate DACA by the current administration, I fulfilled all the pre-med requirements, and I was blessed to get accepted into the University of Utah School of Medicine. I had accomplished something I once thought impossible.
At first, I noticed that my classmates appeared to come from an entirely different background than mine. Being one of the three fully Hispanic students of my class made me question whether I was supposed to be in the same space. Most of my classmates had come from upperclass backgrounds, many of them with mothers, fathers, or both who were physicians. Neither was my case. Just as I was getting over my insecurities, one night destroyed all the confidence I had struggled to build.
After an exhausting day of learning, I stopped at a gas station around 11 p.m. After filling up my tank, I got on the phone with my now-wife and drove off. A couple of seconds later, I saw police lights flashing behind me. I told my now-wife I was getting pulled over and that I would call her back because I did not want her to be worried. I quickly did a mental rundown of anything that would have given them a reason to pull me over. A younger white police officer stood outside my car door, informed me that my headlights were off and asked for my license and registration. I complied. While the officer reviewed my documents, I decided to get some studying done with a phone application that requires me to tap on the screen. When the officer returned, I noticed it was not the same one that had pulled me over. He must have seen my confused look because he started with: “Yeah, I know I am not the same officer that pulled you over.”
“Yeah, I’m confused. What’s going on?” I replied.
“I’m going to need you to step out of the car.”
“Is everything okay?” I asked, feeling my fight or flight response kicking in.
“My partner noticed that you were busy with your hands while he was checking your information. It looked suspicious, so he called me over. I am a K-9 unit narcotics officer and we will check you and your truck for drugs. Do you have any drugs you want to tell me about before we start?”
I was shocked. I did not know what I had done to seem suspicious enough to have an additional K-9 unit over. Maybe I had fidgeted too much with my phone as I was studying? Perhaps the police officer had assumed I did drugs because I was wearing a Mexican Baja jacket. I could blame cultural appropriation for looking “suspicious,” because these jackets are associated with potheads. All I knew was that I had to comply, so I got out of the car. The police officer commanded me to walk toward his vehicle and stand in front of it, facing the windshield. He had me spread my legs and put my hands behind my back. He then proceeded to search me for drugs.
As he was patting me down, he came across my fanny pack. He was having a hard time taking it off with one hand as he held me with his other hand. I attempted to help him, but he forcibly restrained my hands and reminded me not to make any sudden movements. I was instantly reminded of the reality that the situation could quickly escalate if I made any sudden movements that they could perceive as “threatening.” After frisking me, his partner went to get the dog and had it sniff around my truck a couple of times. I was confused, frustrated, and above all, terrified of what the dog’s powerful sense of smell could detect, and I thought that maybe some of the formaldehyde used to preserve the organs from earlier that day could have impregnated my car seat. After they finished, the K-9 unit officer said that the dog had indicated that there may be drugs in the car and that he was going to do a hands-on check. As the officer searched through my stuff, the officer guarding me began questioning me: “So, where are you going?”
“Home,” I said, “I was in school the whole day, and I am tired, so that’s most likely why I forgot to turn my headlights back on.”
“Where do you go to school?” he asked.
“The U,” I replied.
“So, what’s your major?”
“I am in medical school,” I said, hoping that it would positively influence the officer’s judgment of my character.
“Really?” he asked with a raised eyebrow. He must have thought it was a lie because he continued to interrogate me.
“What year?”
“I’m in my first year.”
Still dubious, he asked: “So, how did you get into medical school?”
I could not believe the police officer still doubted me despite the medical student badge I had previously shown him and my water bottle with the School of Medicine’s logo. I felt that I did not need to prove myself worthy of medical school to this police officer. I had already done that to the people who mattered. He must have had his personal biases of why he thought there was no way that someone who looked like me could be in medical school. Reluctantly, I briefed him on the many community service hours, patient exposure, research, clinical employment, leadership roles, and competitive GPA and MCAT score. We were then interrupted by his partner finding my yerba mate. The officer raised it and asked: “What is this?”
“It is a South American herbal tea,” I replied.
“It doesn’t smell like marijuana,” he said sarcastically.
The blatant mistrust in his words heightened my fear. Their determination to view me as a criminal made me afraid that they would find any reason to arrest me. If I got arrested, I would not qualify for DACA anymore, which would make me ineligible for medical school, not to mention being deported. With a prayer in my heart, I mentally went over anything that could potentially give them any reasons for an arrest. Nothing came to mind. Why then, were they treating me as if I was a criminal?
After the search ended and the conversation about what I did in medical school concluded, the officer that was with me said: “The dog sometimes detects lingering smells. If you or someone else smoked some days ago, the dog would still detect it.”
We had just had a conversation about how I was in medical school and I could not do drugs, or I would get kicked out. It still did not matter to them.
“I can’t do drugs. I am in medical school,” I reaffirmed.
As I was walking back to my car, the cop next to me said with a smile: “Well, at least you now have a story to tell.”
I sure did. The police officers thanked me for understanding the “protocol,” and had me wait in my truck. I hoped that I would not get a ticket for having my headlights off on top of everything that they had put me through. I was only given a warning ticket. I drove home feeling humiliated and questioning whether this would be an ongoing part of my life despite any accomplishments I achieve.
The next day, I could not focus on anything. I kept ruminating over the events of the previous night. I was already suffering from “impostor syndrome” from being the only DACA medical student at the University of Utah, so it was not the first time that I had experienced discrimination or racial profiling. However, it was my first time experiencing it as a medical student, and that took me by surprise because I thought I had gotten to a point where people would not question whether I was a productive member of my community. I was wrong.
So, how does one move past such an experience? The police officer was right when he said I had a story to tell. I will tell my story for those who have been racially profiled and lost their lives at the police’s hands. I will tell my story for those who wonder whether they can accomplish their goals and dreams amidst the current political environment. I will tell my story to verify a phrase that a good friend and mentor once said to me: “There are people who are bothered by your mere existence.” We do not have to prove ourselves to anybody but ourselves. We must get to know who we are and what we can accomplish despite society’s biases, prejudices and racist ideologies. These experiences will shape us to be more empathetic servants to those we will serve as professionals.
Despite the traumatic nature of my experience, it helped me realize that I thought of myself the same way those police officers thought of me. I had been feeling out of place just as they felt I was out of place. I did not realize my own headlights had been off during this journey. I have come to terms with the fact that I cannot change people’s minds about what they think of me, but I can change my attitude. I am Mexican, a DACA recipient and a medical student whom God has blessed to be where I am by empowering me to overcome numerous obstacles that have made me a more resilient individual. As other people’s stories are brought to light through social media or articles, this experience has forced me to reflect on my self-perception. My headlights are now on.
How to say I don’t know: A primer on communication for young physicians
First, say I don’t know.
Refuse to apologize. Stand your ground.
Then say I’m sorry.
Defend your sanity and your humanity.
Demand they bow down to the finite
Boundaries of your knowledge
And “appreciate” the distinct contours
Of the discrete, well-circumscribed
Spot, the lesion on the surface of
All that is knowable.
They must tremble in “appreciation”
Of your humility.
If they don’t, repeat I don’t know louder.
Unplug it and plug it back in.
You will find that unless they understand
The deepest depths of your soul,
They will not understand
Your lack of understanding.
And their understanding of this is vital
To your successfully saying I don’t know.
Otherwise, you don’t get the point across.
They won’t know why you don’t know
How you don’t know
What you don’t know.
In which case, you might
Draw a picture of all the things you know.
Use white board markers.
They must be dry erase.
However the drawing only works if it is
Not erased for three days in a row.
The diagrams depict uncertainty
Delicately balanced in negative space
Between red scribbles (for vasculature) and
Scribbles of other colors (for everything else).
And if they find their eyeglasses
Among the tangle of bedsheets and wavering sedatives
Or even if they don’t find those glasses,
They will finally see what you mean
When you say I don’t know.
Montantero
Yellow
Colors have new meaning
since the end of you
My favorite always yellow
is stained by the last breath you drew
Yellow once meant sunshine
when the season changed to fall
now it is the color of your skin and eyes
I think not the death of summer
but instead your suffering
Yellow was the stain on your teeth
one last cigarette
Because smoking meant more to you
than not being dead
Now I have a bag at home and
your bones are the contents inside
The bones sit there
in the dark
but I know
that they are yellow too
Golden Aspens
The Journey
A longing desire,
A burning fire,
A silent journey filled with tears.
We never thought we would have to struggle for so many years!
After countless visits and incoming bills,
After sacrificing so many other thrills,
All the simple solutions have been exhausted.
Through this journey, much of our savings it has costed.
Doctors have said for us the next step is IVF.
We weigh this news against the ever-mounting med school debt.
A reason why, modern medicine does not know.
Thus, on this journey we continue to go.
Many say during medical school it is foolish to try. While their logic is sound, being without makes our hearts cry.
We think “This year we will try with all our might”. Then I hear a classmate joke that a baby is the largest parasite.
We have a special lecture about the benefits of abortion. Oh, what we would give to have their dilemma, even just a portion.
A friend of mine tells me they were blessed to be able to plan. I think to myself, “For us it will happen when it can.”
My class cheers as yet another shouts “I’m excited for my boy!” While happy for them, I wonder when we will feel such joy.
Compared to others we know, this trial seems so small. Yet to me and my spouse, it matters more than all.
Do not underestimate the weight of a trial that has no end. While you cannot relieve my burden, you can be my friend.
Fifteen percent of people struggle to conceive.
We are not alone. We will continue to believe.
This Cold
There is a strange immediacy to the feeling of being cold.
I have spent countless hours in bitter wind and sideways snow, breathless but peaceful in the uphill pursuit of fresh snow, of the drop in my stomach as I bounce off a pillow and feel the cold wet flakes brush my cheeks and let the rest of the world dissolve into white.
But this cold is different.
It’s four thirty in the morning. The bathroom floor is chilly on my bare feet as I rise and sleepily pull scrubs over my head and a brush through my hair. The house we bought in August, a shameless move made in order to somehow create a sense of permanence in this place, does not have great heat up in the attic, and I sleep under two down blankets.
But this cold is different.
It’s five in the morning and my fingers burn as I sacrifice them to the winter, the price of clutching a thermos of warm coffee. I watch my breath precede me in the streetlights as I tiptoe around icy puddles, toes freezing in the clogs that by this time are perfectly molded to my feet after hundreds of hours of walking around the hospital.
But this cold is different.
It’s five thirty. I arrive at the hospital and obediently print patient lists, one for me, one for my resident. She strides in with hand outstretched, silent invisible snarl in her eyes, and snatches it from me without a word. The first time she speaks to me will be after rounds, inevitably a chastisement in the stairwell about my persistent questions or my lingering too long in conversation with a patient.
But this cold is different.
It’s two in the afternoon. I’ve been sent to do a neurological exam on what is known to be a brain dead patient in the SICU. To learn. I gently pull his eyelids up and find non-reactive pupils ringed by icy blue. I hold his snowy white hand.
But this cold is different.
I leave the hospital at eight. It’s snowing out, but I wouldn’t have known, caged as I were inside its walls. I haven’t seen the sunrise or the sunset or the sun in weeks. I’m wearing three layers of coats. My car is being repair and I’m reliant on the train to commute for the first time in my education. It’s a twenty minute walk from the trax stop to my house. I catch my reflection in the glassy black windows. I note with
some degree of apathy that I look tired. A woman sitting opposite me with scraggly teeth talks to herself. There are grocery bags on her feet. She tells me that I have beautiful hair.
I get off the train and I walk home. Still it snows. My path leaves fresh tracks on a fallibly salted sidewalk.
I walk past a small park I’ve driven by every single day for the last seven months, one block from my house. An encampment of homeless tents is clustered there; shopping carts, tarps, and homemade blankets. There’s a little fire. In its patchy light I catch the eye of a woman who looks not older than myself. A long strand of blonde falls out from under her hat and trickles down her cheek. She, too, looks tired.
And this cold is different, because I feel this cold, deeply and in a way that’s less transient, in a way that won’t melt away with a cup of hot tea. I feel the ice in my fingers and the wind cutting through to my jacket right down to whatever is
beneath. I cannot begin to imagine how the yellow haired woman came to be gathered around this fire. Yet the common ground of snow, weather that usually brings me such joy, forcing me to – with jarring immediacy – understand the reality of this world. The other side of the cold. Pins and needles in toes our only similarity and the accident of birth starkly highlighted as I travel home from my cushy doctoral program and realize that I’ve never truly felt the cold. Not like she has.
I pause under a streetlight and watch the snowflakes drift in and out of the shaft of light. It’s silent on the street. On days like this, I usually turn my face to the sky and smile as the tiny hexagons dot my eyelashes. My heart does something I can’t
describe as it falls because snow, for me, has always meant peace. It means something different in this moment. How is that this woman, or one like her, or many like her, has been living a block away from me for seven months and I never knew? How is it that in wishing for the cold and the icy whiteness I was also wishing misery upon her? How did I never pause, before? It is beyond simple to become wrapped up in the safe four walls of the hospital, the complacency of heat and healing. Simple to pour a life into that particular healing so freely that none exists in the cup when you are forced to stop. Simple to lose, in the pursuit of perfection and gratification and education, the ability to see to the humans we once strove to help.
It is much less simple to break out of those four walls.
It is cold outside.
Downtown SLC
Ember
Letter from an MS3 to a brain-dead patient
Dear ZT,
I want to thank you for teaching my what it means to lead a life well lived. I’m sorry we had to meet under these circumstances, but I truly thank you for being such a light in this world.
It’s strange to observe how things work in medicine. My superiors separated themselves from anything that wasn’t your brain, as if distancing ourselves from your life would allow us to provide better medical advice. In the 24 hours we’ve worked on your case, we’ve referred to you under an assumed name and birthdate. I didn’t even know your real name until 5 minutes before we spoke to your family.
When we stepped into the conference room to share the news of your poor prognosis, the sheer number family packed into that small space- 16 in total- made me realize that you were truly loved.
As we started talking about religious needs, your wife wasn’t sure whom to call because YOU were the bishop. This made me realize that you were a man of great consequence, that your story was more than just your brain injury.
When I got home yesterday, I started looking you up online. And suddenly you became more than a limp body in a hospital bed and a damaged brain on a computer screen. I learned that you were a leader in the business community, passionate about serving others, and that your life philosophy was to take calculated risks in order to live life to the fullest.
We met at a curious time in our lives- mine just beginning as yours is just ending. However, if there’s any consolation from our encounter, it’s that learning more about you has taught me that I cannot continue to live life without striving to be the best person I can be.
I’ll be honest, medical school has been tough. Over the last few months, I’ve been questioning why I even pursued this path in the first place: Was it to please my parents? Was it to find financial stability? Was it to advance in society?
Learning about you- and not just your brain- has made me understand that medicine is my calling. Thank you for teaching me that being in medicine is truly an amazing privilege. Because I chose medicine, I get to experience people, society, and life on a level deeper than any other career.
Before, I might have said that you’re the kind of man I can only dream of becoming one day. This morning I finally realized “that day” is today. The future is what we make of it and I owe it to you to strive to become the best doctor and person I can be.
Thank you so much.
Sincerely,
Jason Chen
Separation of Patient and Family
I grew up understanding the concept of separation of church and state, and as I grew up in the medical profession I soon learned about the concept of separation of patient and family. As a young nurse in the Emergency Department I was shocked when a full arrest came through the ambulance doors and the wife of 60 years was rushed into a corner of the waiting room while she
waited for someone to update her on his condition. I worked with one physician who had absolutely no interest in talking to the family so when he was working I became the bearer of bad news. I always felt it was so sterile and inappropriate to have the one person who cared the most about the just another “full arrest” on the gurney in the other room, sitting in a corner, often times, all alone.
The general wisdom at that time was to give periodic updates where you “primed the pump” so to speak. We learned to use phrases that were practically memorized, “We are doing everything we can for them right now, they have the very best care and resources working on them, he hasn’t responded to our treatments so far, but we are continuing to try, we are hoping the next round of medications will stimulate his heart etc.” You will notice the complete and absolute absence of the word “dead” but more importantly no mention of “what would they have wanted in this situation, or have you talked about resuscitation efforts with your loved one?” Sometimes, even after we had stopped resuscitative efforts, we would go out to the waiting room and offer further information indicating we were still working on them. This was all designed to give them time to accept what was often the inevitable. The folly in this is the actual belief that waiting another 10 minutes to tell them their loved one is dead would ease them into this shocking news. There we go again, thinking as medical professionals we could affect and or control human emotions to the most devastating news they would ever receive. Eventually we would inform them that our efforts were unsuccessful (without mentioning what those efforts were) and inform them their loved one had _______fill in the blank with whatever word makes you feel better. Again, we felt we could soften the blow by using more acceptable terms including “passed away, failed to respond.” As I write this I am astounded at how inappropriate, archaic and delusional our thought processes were. We may have tried to find a quiet place to talk to the family but often we were forced to go through this whole dance in the corner of the emergency room waiting room.
What happened next was very team specific – should we let them in the room to see the body? The prevailing thought was that it would probably be best to wait to see them in the more controlled setting of the mortuary, especially if they were a coroner’s case and we were required to leave all the medical devices in place, the IVs, the arterial lines, the endotracheal tubes etc. This practice was severely challenged one night as a young adult male was brought in by paramedics to the ER. He was sitting behind the driver of a motorcycle when a sudden stop sent him flying onto the car in front of them and his neck was sliced open down to his sternum from the sharp edged rain gutter that used to adorn cars. His eyes were open, his mouth was open while his tongue had been cut in half by his teeth. It was shocking for all of us to see.
A few hours later, a woman arrived indicating she had heard that her son may have possibly been brought in from a motorcycle accident. We finally established that the John Doe in the back room was in fact her son. I showed her his identification we had found in his wallet and she was stoic. I explained there was significant trauma involved and that it would be best to see him at the mortuary. She left. She returned. She left, and she returned three more times, always with
essentially the same dialogue. Finally, she implored that she needed to see him, because “I just can’t believe it’s really him and that he’s really dead.” Silence. I asked for a few moments and did my best to cover up the gaping holes in his neck and chest. I had unsuccessfully tried to close his eyes earlier. I prepared her for what she was about to see, and took her back to be with her son. She wept, instinctively my arm was around her. She whispered “it really is him. Thank you.” She survived, and had taught me, a young nurse, a most valuable lesson. I really didn’t know what was best for her.
Gratefully institutions began exploring the presence of family members during resuscitation and procedures, especially in the pediatric population that eventually spread to adult patients. The literature is replete with favorable and studied rationale behind this practice, despite some practitioners still swimming against the tide. With this newly acquired enlightenment many practices started going by the wayside including strict limited visiting hours, age restrictions on visitors, allowing more than 2 people in the room at the same time and forbidding anything that resembled or tasted like home into the hospital.
I arrived at a small community hospital in Orange County, California to transport a 64 year-old male patient with a dissecting thoracic aortic aneurysm. The helicopter flight was only 12 minutes, but the preparation and loading process would take significantly longer. His blood pressure was dropping quickly as the dissection extended. Pharmacological interventions to reduce the pressure and drop the heart rate had proven ineffective. As is often the case, the staff had scattered, grateful for our arrival and the reprieve from caring for a patient typically out of their comfort zone. His construction worker son was seated next to him, fresh from a muddy job as evidenced by the mud on the floor and his boots. He appeared to have no idea how sick his dad was. It soon became clear that he would not survive the flight. By now he was profoundly bradycardic and hypotensive enough to require a Doppler to get the pressure. He was drifting in and out of consciousness and his distal pulses were absent. I pulled up a stool and talked to them both about the seriousness of his condition and the options we had before us. We could load him and fly him to the receiving University hospital with the high probability that he would go into full arrest and require resuscitation and likely not survive to get to the operating room. Or, we could sit with him, and allow his son to be with him and allow him to die in as peaceful a way as possible. His son quickly chose the latter.
I remained with them, and encouraged the son to lean down, touch his dad and tell him those things he wanted to say. I was honored to witness a most poignant and tender scene as this burly construction worker wept as he apologized for his teen age antics, for his absence during his rebellious years and professed his absolute love and admiration for his dad who had provided a safe and loving life for him. As his heart neared asystole, I asked if he wanted us to start resuscitation efforts that would include medications and CPR. He looked up and shook his head in the affirmative. His son kept talking into his dad’s ear, apparently there were more sentiments he needed to express. After five minutes, I asked again and this time, he simply said “No, I am ready to let him go now.” I was moved and as we hugged, tears flowed. I was humbled by what had just transpired and grateful that we had moved far from the days of separation of family and patient.
Patients’ families relive the worst day of their life over and over. They replay our actions, our attitudes, our facial expressions, their feelings and their feelings about us, as caregivers. They talk about “that day” at family get togethers, and at holidays. It’s vital to continually assess whether we are merely health care providers, or we are caregivers. For me, I want caregivers on my family members’ team. I want caregivers who follow the theory of relativity, where they treat patients like they are their relative, for they are indeed someone’s mother, wife, sister, daughter… I wouldn’t want my mom to die in the presence of only strangers, or to have all decision making left in the hands of those strangers, or to not have her pain addressed at consistent intervals, or fail to recognize that she is and was a vital and vibrant woman who contributed much to the world. True caregivers will do all of that and more.
oh my God! – it’s full of stars!

This photo of my wife Paula K. Rudd, of 27 years, circa 2016, was taken through the side-glass window of our car on a rainy afternoon. Her hair is sprouting after completing stage 4 breast cancer chemo regime, a mastectomy, a lymphadenectomy of 14 nodes, 12-week radiation, and reconstruction surgery (twice). She survives today. Even as recently as 2020, she was diagnosed with a metastasized reoccurance near her bladder. 9-months of bilateral nephrostomy tubes, and another successful response to treatment. Her hair is sprouting again.
This work combines references to: the title of the piece is from a scene in “2001 – A Space Odyssey”, a quote “We’re made of star stuff” by Carl Sagan, and iconography religious paintings from the middle ages of saints with halos. Like the French “Realists” of the 1800’s, questioning the “nobility of subject matter worthy of creation”; Truth, Veritas, raw, unadorned, needs no approval. Bestowing sainthood is no longer reserved to the priestly class.
Haunted
I am haunted
Followed by a ghost down bustling hospital hallways
It is drawn to the white coat that wears me
I see glimpses of its shadow in the yellowing of a patient’s skin and the rasp of smoker’s cough
The ghost draws my attention to common items in hospital rooms
The texture of a chair so painfully familiar beneath my fingertips
The fabric pattern makes my gut clench and eyes water
I hear whispers hidden in the white noise of oxygen tubing and alarming IV’s
Hidden in the darkness, I carry with me
~Sweetheart, have I told you how much I love you today? ~
Tears soak my cheeks
I wish I could disappear, but my white coat is bright and blinding
I leave the room, head down and gasping for breath
Sinking to my knees in the first place I find empty, sobs escaping
“No, Dad… you haven’t, how much do you love me?”
The response is silence
But still, I am haunted
The memory a man with his hands held wide, saying “this much!” unrelenting